Building a Healthy World for All
At York University’s Faculty of Health, we are striving in all we do to be leaders and partners for a healthy and just 21st century world.
Our six degree programs — Global Health, Health Studies (Policy, Management, Digital Health), Kinesiology & Health Science, Neuroscience, Nursing and Psychology — expand our understandings of health, bring innovations to health education, and contribute to the wellbeing of people and communities all around the world.
Through our teaching and research excellence, and with our community partners — locally and globally — we are acting every day to build a healthy world for all. Because we believe health is a fundamental human right. For everyone.

Congratulations to Distinguished Research Professor in Psychology and Officer of the Order of Canada, Debra Pepler, one of Canada's foremost researchers and experts on youth bullying and aggression, on her election to the Royal Society of Canada in recognition of her career achievements and contributions to public life.

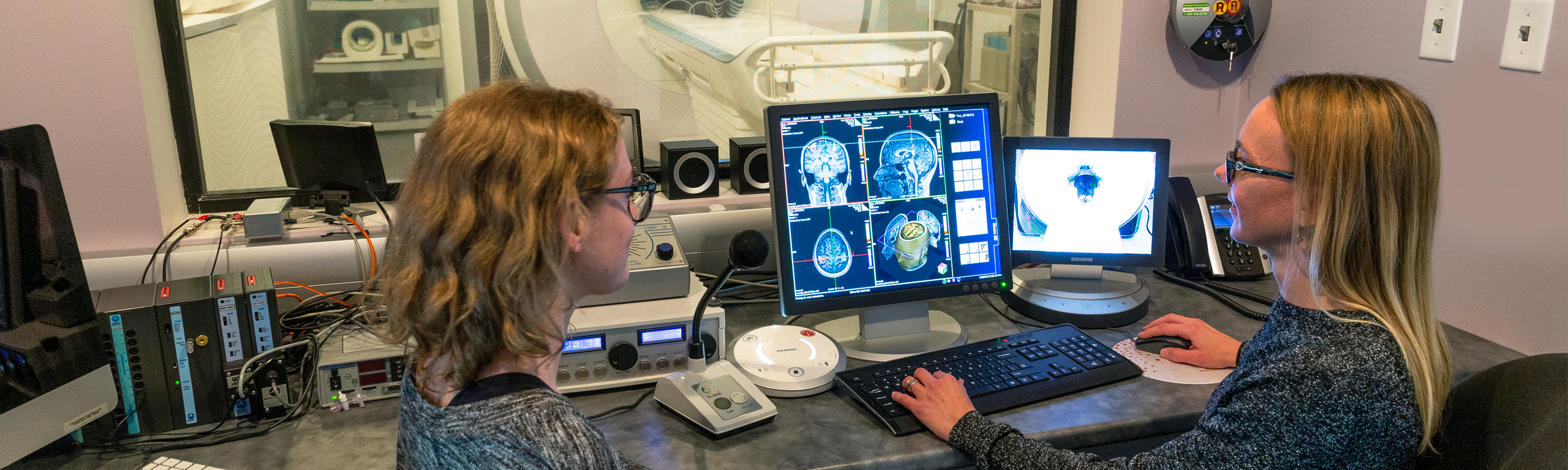
In a newly published paper on Artificial intelligence-based computer aided detection (AI-CAD) in the fight against tuberculosis, Global Health Professor Amrita Daftary says the risk of using AI-CAD could reduce the fight against TB to one that is purely technical and technological, while neglecting its social determinants and effects.

MEET THE CHANGEMAKERS
Learn more about Faculty of Health students, alumni, faculty and staff who are creating positive change.

STUDENT SUCCESS PROGRAMS
Explore peer mentorship, leadership and development, and peer assisted learning programs for students in the Faculty of Health.

ADVANCING QUALITY EDUCATION
Get more information on how we support student learning in the Faculty of Health.
Events
YorkU Health
Programs
Undergraduate Programs
Undergraduate programs in Global Health, Health Studies, Kinesiology & Health Science, Nursing, Neuroscience, and Psychology
Graduate Programs
Graduate programs in Health, Critical Disability Studies, Global Health, Kinesiology & Health Science, Nursing, and Psychology

TEACHING SPOTLIGHT
“Life-changing” learning at York’s Costa Rica EcoCampus
AFTER TAKING AN IMMERSIVE, community based field course at York’s Las Nubes EcoCampus in Costa Rica, associate professor of Psychology and environmentalist Adrienne Perry knew she wanted to become more involved.